Does Mammoplasty Impair The Breastfeeding Function?
One of the most frequently asked questions by candidates considering mammoplasty but also becoming a mother and breastfeeding their baby is whether mammoplasty has a negative impact on breastfeeding function.
In this article, I wanted to look at the lactation function and discuss how a variety of mammoplasty procedures affect lactation.
For the infant to be nourished after delivery through breastfeeding, many anatomical structures and hormonal elements must be in good condition and functioning. Through 12-20 milk ducts, the milk glands in the mammary tissue open to the holes in the nipple. When the baby starts sucking the nipple, the brain is stimulated and release hormones associated with lactation.
With the effect of these hormones, milk is produced and previously produced milk is pumped towards the nipple through contraction of the mammary glands.
To summarize in the simplest words; it is essential that the baby sucks nipple, there is a nipple that the baby can suck, sensory nerves in the nipple are intact and can transmit the baby’s sucking stimulus to the brain, hormones for milk production are secreted appropriately in the brain, the mammary glands are healthy and can produce milk, the milk ducts that carry the milk produced in the mammary glands to the nipple are adequate and open, and the holes in the nipple to where the milk ducts open are adequate and open.
Any problem in the anatomical structures mentioned above (nipple, mammary gland, and milk ducts) or in the hormone secretion system may impair the lactation function. I want to emphasize here that there is no rule that every mother has to breastfeed her baby.
The breastfeeding function may be impaired due to a variety of factors. It should be noted that if a woman who has never experienced a lactation period before has a baby after a mammoplasty operation and discovers that she is unable to breastfeed, the mammoplasty operation alone cannot be held responsible for this inability. Perhaps this woman wouldn’t be able to breastfeed her baby even if she didn’t have mammoplasty.
Let’s take a closer look at the relationship between mammoplasty and the lactation – breastfeeding function in light of this preliminary information. A mammoplasty operation does not impair the lactation function as long as the nipple sensation is maintained and the relationship between the nipple and an adequate number of mammary glands as well as the milk ducts is preserved as a whole.
As is well known, the term “mammoplasty” does not refer to a single surgical procedure; instead, it refers to a variety of surgical procedure intended to improve the aesthetic appearance of the breast. The primary ones among these are breast augmentation with silicone implant, breast lift, breast augmentation plus breast lift, and breast reduction.
Breast Augmentation Surgery and Lactation — Breastfeeding
In this procedure, a pouch is created completely beneath the breast tissue and a silicone implant is placed in it. Since the procedure does not involve direct intervention in the mammary tissue, it is not expected to impair the lactation function.
Especially if the pocket is prepared by accessing the target area through an incision made in the inframammary fold or armpit, the breast tissue is not involved by the intervention in any way, and therefore the procedure carries no risk.
The technique, which allows for accessing the breast tissue through an incision made in the areola, carries the risk of damaging the nerves around the nipple, but this happens very rarely.
Excessive stretching, on the other hand, may rarely result in permanent damage to the nerves that provide the sensation of the nipple. Such a condition may cause a problem in the transmission of the baby’s sucking sensation to the brain.
Breast Lift and Lactation — Breastfeeding
Breast lift surgery involves the use of a variety of surgical techniques depending on the degree of sagging and deformation in the breast. The excess breast skin is removed three-dimensionally, the nipple is elevated to a higher point, and the breast is reshaped to achieve a more aesthetic appearance.
In some techniques, the breast tissue is repositioned by making incisions on a portion of it. In general, because breast lift surgery does not involve the milk glands or milk ducts, it carries no significant risk to the breastfeeding function. The same can be said about t breast augmentation plus breast lift surgery.
Breast Reduction and Lactation — Breastfeeding
“Breast reduction” the mammoplasty procedure that is known to carry the highest risk of impairing the lactation (breastfeeding) function, and it is being questioned due to this. While breast reduction surgery removes some of the breast tissue that has grown to be too large due to various factors, the amount of breast tissue required in a normal breast is left in place.
The lactation (breastfeeding) function is maintained by preserving the remaining breast tissue as a whole with the mammary glands, milk ducts and the connection of these ducts with the nipple. This is taken into account in today’s surgical techniques, and special attention is paid to the protection of the lactation (breastfeeding) function.
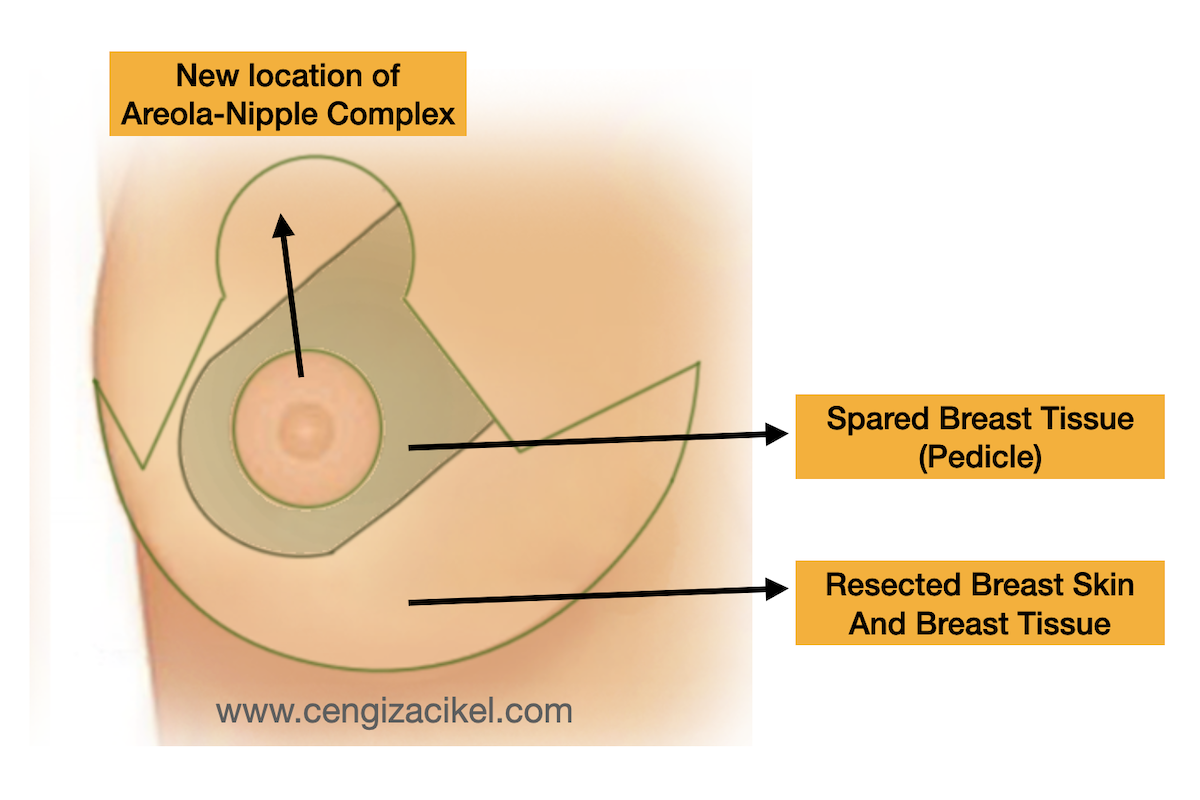
As shown in the image, the nipple and the pigmented area (areola) around it are preserved as a block with the breast tissue under it. The size of the preserved breast tissue is determined based on body and breast measurements.
This structure, known as a pedicle, can have different designs depending on the surgical technique used, but they all are intended to protect the lactation (breastfeeding function).
In a surgical technique used to reduce extremely large and sagging breasts, the nipple and the pigmented skin around it known as the nipple-areola complex are removed by disconnecting it from the milk ducts at the beginning of the surgery, and after the completion of the breast reduction operation, this part is sutured in its new place as a patch.
Since the milk ducts are completely cut in this technique known as the free nipple graft technique, the lactation (breastfeeding) function is expected to be impaired. This technique that was more common in the past is now rarely used.
Especially for women are planning to have a baby, techniques that preserve the lactation (breastfeeding) function are preferred.
Nipple Reduction Surgery and Lactation — Breastfeeding
Women with larger-than-normal nipples demand nipple reduction surgery for aesthetic reasons.
In some surgical techniques used for this purpose, the milk ducts opening to the nipple are cut to a considerable extent, while they are tried to be preserved in some other techniques.
In my practice, I advise women who consider breastfeeding their babies to postpone the nipple reduction surgery until the completion of all the current and expected pregnancy and breastfeeding periods.
I emphasize the importance of the nipple for the baby’s sucking function and state that a large nipple can even be an advantage for the baby. I also state that the milk ducts may be damaged even if a surgical technique that preserves the milk ducts is used.
Areola Reduction Surgery and Lactation — Breastfeeding
In some cases, the pigmented circular part (areola) around the nipple can be larger than normal and asymmetrical. The areola reduction procedure, which involves removing a donut-shaped piece of skin, has no serious side effects on the lactation (breastfeeding) function.
Conclusion
The risk is not zero in mammoplasty procedures, although the lactation (breastfeeding) function is carefully preserved. On the written consent forms given to you before the operation, you can see that no guarantee is given to you in this regard.
Therefore, I recommend that you discuss such concerns with your physician during the preoperative interview of the planned mammoplasty operation, learn about the risks of the surgical technique to be used, and then make a decision accordingly.
Another point I’d like to emphasize is that women who have previously had a mammoplasty operation and were unable to breastfeed their babies should know that they might still be unable to breastfeed their babies even if they did not have the mammoplasty operation. Even under normal conditions, the mother may be unable to breastfeed her baby due to anatomical and hormonal factors.
References:
- Infant and Young Child Feeding: Model Chapter for Textbooks for Medical Students and Allied Health Professionals. Geneva: World Health Organization; 2009.